
Back Hipertensie AF ارتفاع ضغط الدم Arabic ارتفاع ضغط الدم ARZ উচ্চ ৰক্তচাপ AS Hipertensión arterial AST Arterial hipertenziya AZ یوخاری قان فیشاری AZB Гипертония BA Bluadhochdruck BAR Артэрыяльная гіпертэнзія BE
| Hypertension | |
|---|---|
| Other names | Arterial hypertension, high blood pressure |
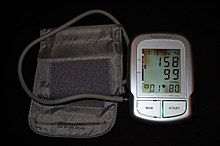 | |
| Automated arm blood pressure meter showing arterial hypertension (shown by a systolic blood pressure 158 mmHg, diastolic blood pressure 99 mmHg and heart rate of 80 beats per minute) | |
| Specialty | Cardiology |
| Symptoms | None[1] |
| Complications | Coronary artery disease, stroke, heart failure, peripheral arterial disease, vision loss, chronic kidney disease, dementia[2][3][4] |
| Causes | Usually lifestyle and genetic factors[5][6] |
| Risk factors | Lack of sleep, excess salt, excess body weight, smoking, alcohol,[1][5] air pollution[7] |
| Diagnostic method | Resting blood pressure 130/80 or 140/90 mmHg[5][8] |
| Treatment | Lifestyle changes, medications[9] |
| Frequency | 16–37% globally[5] |
| Deaths | 9.4 million / 18% (2010)[10] |
| Part of a series on |
| Human body weight |
|---|
Hypertension, also known as high blood pressure, is a long-term medical condition in which the blood pressure in the arteries is persistently elevated.[11] High blood pressure usually does not cause symptoms itself.[1] It is, however, a major risk factor for stroke, coronary artery disease, heart failure, atrial fibrillation, peripheral arterial disease, vision loss, chronic kidney disease, and dementia.[2][3][4][12] Hypertension is a major cause of premature death worldwide.[13]
High blood pressure is classified as primary (essential) hypertension or secondary hypertension.[5] About 90–95% of cases are primary, defined as high blood pressure due to nonspecific lifestyle and genetic factors.[5][6] Lifestyle factors that increase the risk include excess salt in the diet, excess body weight, smoking, physical inactivity and alcohol use.[1][5] The remaining 5–10% of cases are categorized as secondary high blood pressure, defined as high blood pressure due to a clearly identifiable cause, such as chronic kidney disease, narrowing of the kidney arteries, an endocrine disorder, or the use of birth control pills.[5]
Blood pressure is classified by two measurements, the systolic (high reading) and diastolic (lower reading) pressures.[1] For most adults, normal blood pressure at rest is within the range of 100–130 millimeters mercury (mmHg) systolic and 60–80 mmHg diastolic.[8][14] For most adults, high blood pressure is present if the resting blood pressure is persistently at or above 130/80 or 140/90 mmHg.[5][8] Different numbers apply to children.[15] Ambulatory blood pressure monitoring over a 24-hour period appears more accurate than office-based blood pressure measurement.[5][11] Hypertension is around twice as common in diabetics.[16]
Lifestyle changes and medications can lower blood pressure and decrease the risk of health complications.[9] Lifestyle changes include weight loss, physical exercise, decreased salt intake, reducing alcohol intake, and a healthy diet.[5] If lifestyle changes are not sufficient, then blood pressure medications are used.[9] Up to three medications taken concurrently can control blood pressure in 90% of people.[5] The treatment of moderately high arterial blood pressure (defined as >160/100 mmHg) with medications is associated with an improved life expectancy.[17] The effect of treatment of blood pressure between 130/80 mmHg and 160/100 mmHg is less clear, with some reviews finding benefit[8][18][19] and others finding unclear benefit.[20][21][22] High blood pressure affects between 16 and 37% of the population globally.[5] In 2010 hypertension was believed to have been a factor in 17.8% of all deaths (9.4 million globally).[10]
- ^ a b c d e "High Blood Pressure Fact Sheet". CDC. 19 February 2015. Archived from the original on 6 March 2016. Retrieved 6 March 2016.
- ^ a b Lackland DT, Weber MA (May 2015). "Global burden of cardiovascular disease and stroke: hypertension at the core". The Canadian Journal of Cardiology. 31 (5): 569–571. doi:10.1016/j.cjca.2015.01.009. PMID 25795106.
- ^ a b Mendis S, Puska P, Norrving B (2011). Global atlas on cardiovascular disease prevention and control (PDF) (1st ed.). Geneva: World Health Organization in collaboration with the World Heart Federation and the World Stroke Organization. p. 38. ISBN 978-92-4-156437-3. Archived from the original (PDF) on 17 August 2014.
- ^ a b Hernandorena I, Duron E, Vidal JS, Hanon O (July 2017). "Treatment options and considerations for hypertensive patients to prevent dementia". Expert Opinion on Pharmacotherapy (Review). 18 (10): 989–1000. doi:10.1080/14656566.2017.1333599. PMID 28532183. S2CID 46601689.
- ^ a b c d e f g h i j k l m Poulter NR, Prabhakaran D, Caulfield M (August 2015). "Hypertension". Lancet. 386 (9995): 801–812. doi:10.1016/s0140-6736(14)61468-9. PMID 25832858. S2CID 208792897.
- ^ a b Carretero OA, Oparil S (January 2000). "Essential hypertension. Part I: definition and etiology". Circulation. 101 (3): 329–335. doi:10.1161/01.CIR.101.3.329. PMID 10645931.
- ^ Yang BY, Qian Z, Howard SW, Vaughn MG, Fan SJ, Liu KK, Dong GH (April 2018). "Global association between ambient air pollution and blood pressure: A systematic review and meta-analysis". Environmental Pollution. 235: 576–588. Bibcode:2018EPoll.235..576Y. doi:10.1016/j.envpol.2018.01.001. PMID 29331891.
- ^ a b c d Whelton PK, Carey RM, Aronow WS, Casey DE, Collins KJ, Dennison Himmelfarb C, DePalma SM, Gidding S, Jamerson KA, Jones DW, MacLaughlin EJ, Muntner P, Ovbiagele B, Smith SC, Spencer CC, Stafford RS, Taler SJ, Thomas RJ, Williams KA, Williamson JD, Wright JT (June 2018). "2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines". Hypertension. 71 (6): e13–e115. doi:10.1161/HYP.0000000000000065. PMID 29133356.
- ^ a b c "How Is High Blood Pressure Treated?". National Heart, Lung, and Blood Institute. 10 September 2015. Archived from the original on 6 April 2016. Retrieved 6 March 2016.
- ^ a b Campbell NR, Lackland DT, Lisheng L, Niebylski ML, Nilsson PM, Zhang XH (March 2015). "Using the Global Burden of Disease study to assist development of nation-specific fact sheets to promote prevention and control of hypertension and reduction in dietary salt: a resource from the World Hypertension League". Journal of Clinical Hypertension. 17 (3): 165–167. doi:10.1111/jch.12479. PMC 8031937. PMID 25644474. S2CID 206028313.
- ^ a b Naish J, Court DS (2014). Medical sciences (2 ed.). Elsevier Health Sciences. p. 562. ISBN 978-0-7020-5249-1.
- ^ Lau DH, Nattel S, Kalman JM, Sanders P (August 2017). "Modifiable Risk Factors and Atrial Fibrillation". Circulation (Review). 136 (6): 583–596. doi:10.1161/CIRCULATIONAHA.116.023163. PMID 28784826.
- ^ "Hypertension". World Health Organization. Retrieved 13 May 2022.
- ^ Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Böhm M, et al. (July 2013). "2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC)". European Heart Journal. 34 (28): 2159–2219. doi:10.1093/eurheartj/eht151. hdl:1854/LU-4127523. PMID 23771844.
- ^ James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, Handler J, Lackland DT, LeFevre ML, MacKenzie TD, Ogedegbe O, Smith SC, Svetkey LP, Taler SJ, Townsend RR, Wright JT, Narva AS, Ortiz E (February 2014). "2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8)". JAMA. 311 (5): 507–520. doi:10.1001/jama.2013.284427. PMID 24352797.
- ^ Petrie JR, Guzik TJ, Touyz RM (May 2018). "Diabetes, Hypertension, and Cardiovascular Disease: Clinical Insights and Vascular Mechanisms". The Canadian Journal of Cardiology. 34 (5): 575–584. doi:10.1016/j.cjca.2017.12.005. PMC 5953551. PMID 29459239.
- ^ Musini VM, Tejani AM, Bassett K, Puil L, Wright JM (June 2019). "Pharmacotherapy for hypertension in adults 60 years or older". The Cochrane Database of Systematic Reviews. 6 (6): CD000028. doi:10.1002/14651858.CD000028.pub3. PMC 6550717. PMID 31167038.
- ^ Sundström J, Arima H, Jackson R, Turnbull F, Rahimi K, Chalmers J, Woodward M, Neal B (February 2015). "Effects of blood pressure reduction in mild hypertension: a systematic review and meta-analysis". Annals of Internal Medicine. 162 (3): 184–191. doi:10.7326/M14-0773. PMID 25531552. S2CID 46553658.
- ^ Xie X, Atkins E, Lv J, Bennett A, Neal B, Ninomiya T, Woodward M, MacMahon S, Turnbull F, Hillis GS, Chalmers J, Mant J, Salam A, Rahimi K, Perkovic V, Rodgers A (January 2016). "Effects of intensive blood pressure lowering on cardiovascular and renal outcomes: updated systematic review and meta-analysis". Lancet. 387 (10017): 435–443. doi:10.1016/S0140-6736(15)00805-3. PMID 26559744. S2CID 36805676. Archived from the original on 16 April 2019. Retrieved 11 February 2019.
- ^ Diao D, Wright JM, Cundiff DK, Gueyffier F (August 2012). "Pharmacotherapy for mild hypertension". The Cochrane Database of Systematic Reviews. 8 (8): CD006742. doi:10.1002/14651858.CD006742.pub2. PMC 8985074. PMID 22895954. S2CID 42363250.
- ^ Garrison SR, Kolber MR, Korownyk CS, McCracken RK, Heran BS, Allan GM (August 2017). "Blood pressure targets for hypertension in older adults". The Cochrane Database of Systematic Reviews. 2017 (8): CD011575. doi:10.1002/14651858.CD011575.pub2. PMC 6483478. PMID 28787537.
- ^ Musini VM, Gueyffier F, Puil L, Salzwedel DM, Wright JM (August 2017). "Pharmacotherapy for hypertension in adults aged 18 to 59 years". The Cochrane Database of Systematic Reviews. 2017 (8): CD008276. doi:10.1002/14651858.CD008276.pub2. PMC 6483466. PMID 28813123.